For decades, Parkinson’s disease has been primarily understood as a movement disorder. When we think of Parkinson’s, we typically picture tremors, stiffness, and difficulty walking. Medical science largely attributed these symptoms to a lack of dopamine and dysfunction in a specific, deep part of the brain called the basal ganglia.
However, this traditional view has always left crucial questions unanswered. Patients frequently experience a wide range of non-motor symptoms, including sleep disturbances, digestive issues, anxiety, and cognitive decline, often years before movement problems appear. How could a localized motor defect explain all of this?
Our recent research, published in Nature, fundamentally shifts this paradigm. By analyzing a massive dataset of brain imaging from 863 individuals, we discovered that Parkinson’s disease is rooted in a much broader network dysfunction. It is not just a localized problem, but a disorder of a newly identified brain system known as the somato-cognitive action network (SCAN).
The SCAN is a critical network within the brain’s motor cortex that links action planning with bodily functions. It physically connects our cognitive intentions, whole-body movements, and internal organ physiology. In our study, we found that in individuals with Parkinson’s disease, the SCAN becomes abnormally hyperconnected to the subcortex, the deep brain relay center. This excessive “wiring” disrupts not only voluntary movement but also the related cognitive and bodily functions that the SCAN controls.
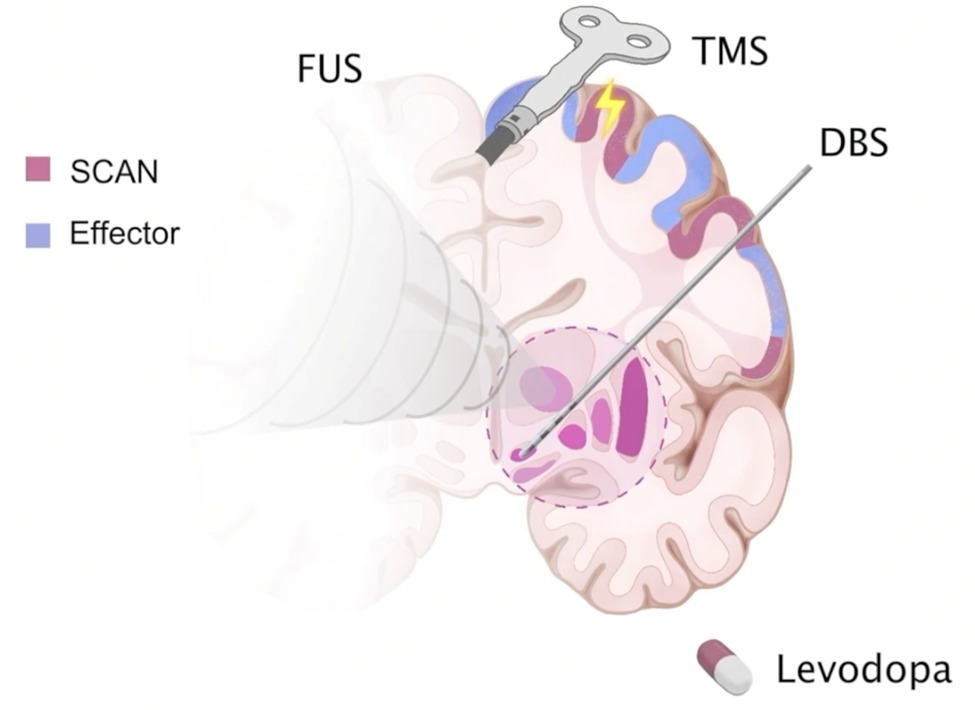
This discovery changes everything about how we understand and treat the disease. We observed that existing therapies, such as Levodopa medication and Deep Brain Stimulation (DBS), actually work by reducing this exact hyperconnectivity between the SCAN and the subcortex. Furthermore, when we used an exploratory clinical study of transcranial magnetic stimulation (TMS) to precisely target the SCAN in patients, their symptom showed highly significant improvement compared to traditional targeting methods.
By redefining Parkinson’s as a SCAN disorder, we can shift our focus from treating a scattered collection of symptoms to addressing the core circuit pathology. This offers immense hope for the future. It means we can develop highly personalized, precise interventions targeted directly at the SCAN, potentially treating Parkinson’s disease more successfully than was ever previously possible.
Reference
- Ren, J., Zhang, W., Dahmani, L. et al. Parkinson’s disease as a somato-cognitive action network disorder. Nature (2026). https://doi.org/10.1038/s41586-025-10059-1
Jianxun Ren is a principal investigator at Changping Laboratory, Beijing, China, and a visiting scholar at Harvard Medical School. He received his B.Eng. and Ph.D. from Tsinghua University. Driven by the goal of translating advanced imaging techniques into precise therapies, his research focuses on precision brain functional imaging and neuromodulation. He has published more than 40 peer-reviewed scientific papers, with 18 as first or corresponding author in prestigious journals including Nature, Nature Methods, Nature Neuroscience, Nature Communications, Annals of Neurology, and Brain Stimulation.